Your Home BP Guide
A quick reference for taking accurate blood pressure readings during pregnancy
Want the full details? Read our complete step-by-step guide or download the Connura Home BP Guide
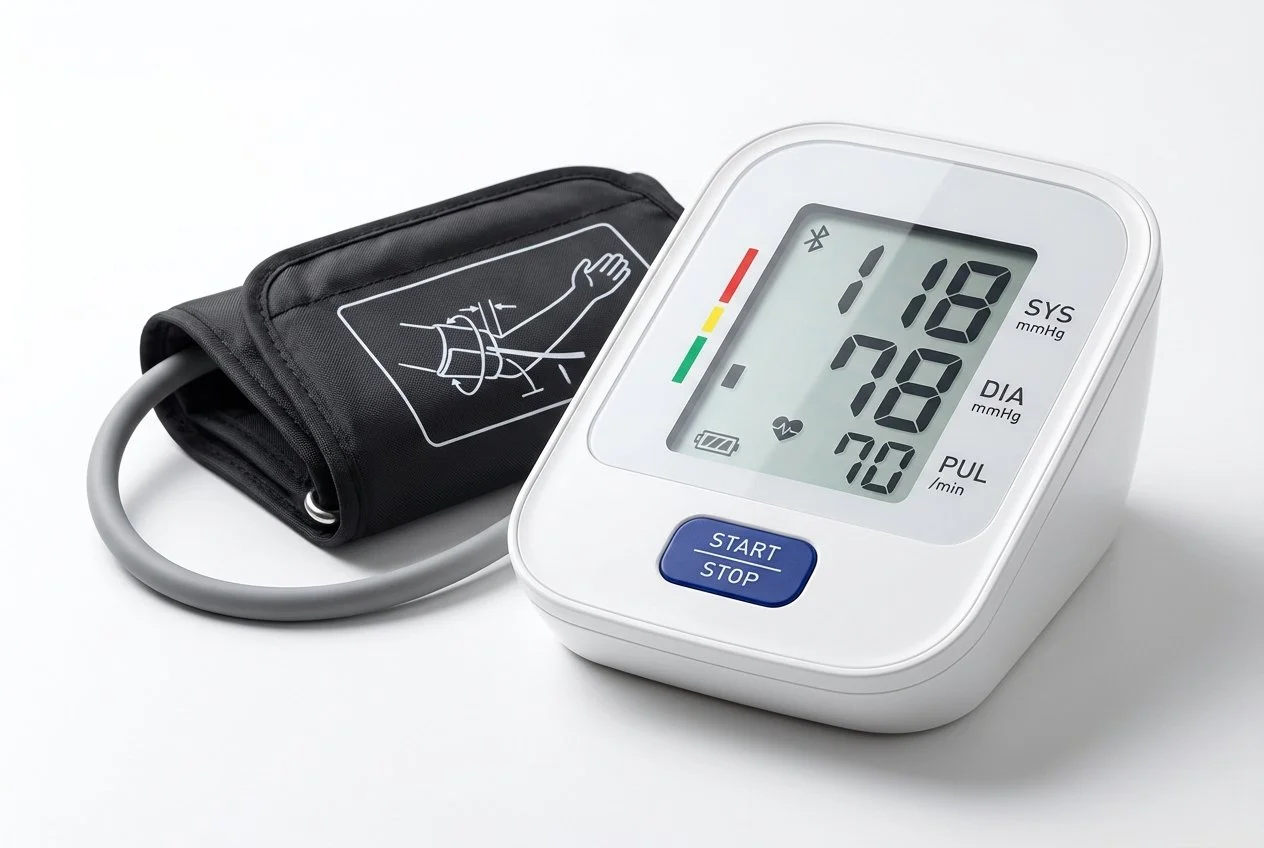
Use the Right Monitor
Not all monitors are equal — and the right setup makes your readings more reliable.
Use an automatic, upper-arm cuff monitor. Wrist and finger monitors are not recommended for clinical accuracy.
Check that your monitor is validated. Your provider can recommend one, or you can check validatebp.org for tested devices.
Make sure the cuff fits. A cuff that's too small or too large can shift your reading by as much as 30 points. Most monitors come with a standard cuff — if your arm measures larger than 13 inches around, ask about a large adult cuff.
Re-check the fit as your pregnancy progresses. Your arm size can change — a cuff that fit in your second trimester may not fit the same in your third.
If you're not sure whether your monitor or cuff size is right, bring it to your next appointment. Your care team can check it with you.
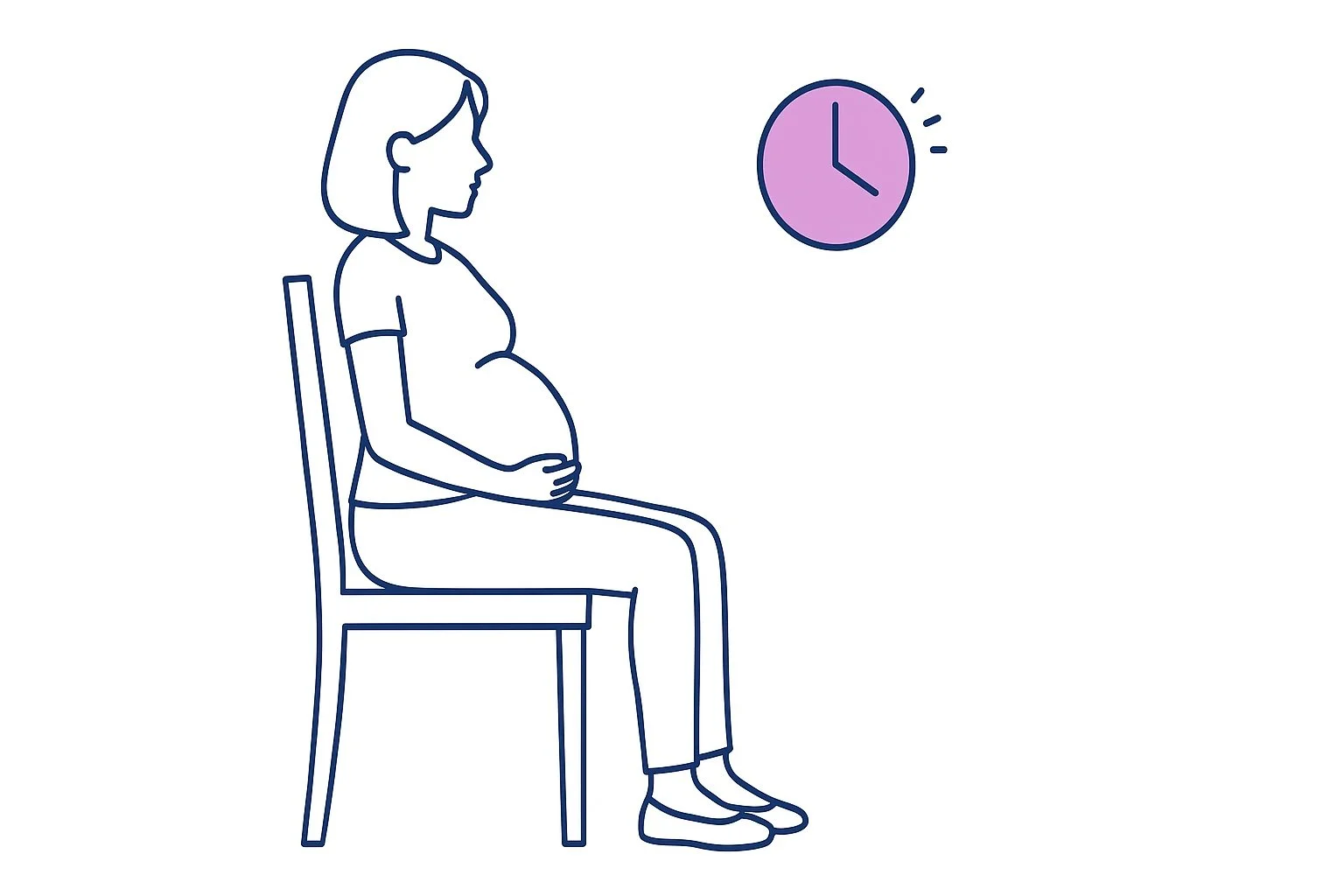
Before You Measure
Sit quietly for 5 minutes — set a timer, let your body settle
Empty your bladder
No caffeine for 30 minutes before your reading
Don't measure right after activity or stress
Why the 5-minute rest matters: Your blood pressure naturally fluctuates throughout the day. Sitting quietly first gives you a baseline that your care team can actually use — not a reading driven by what just happened.
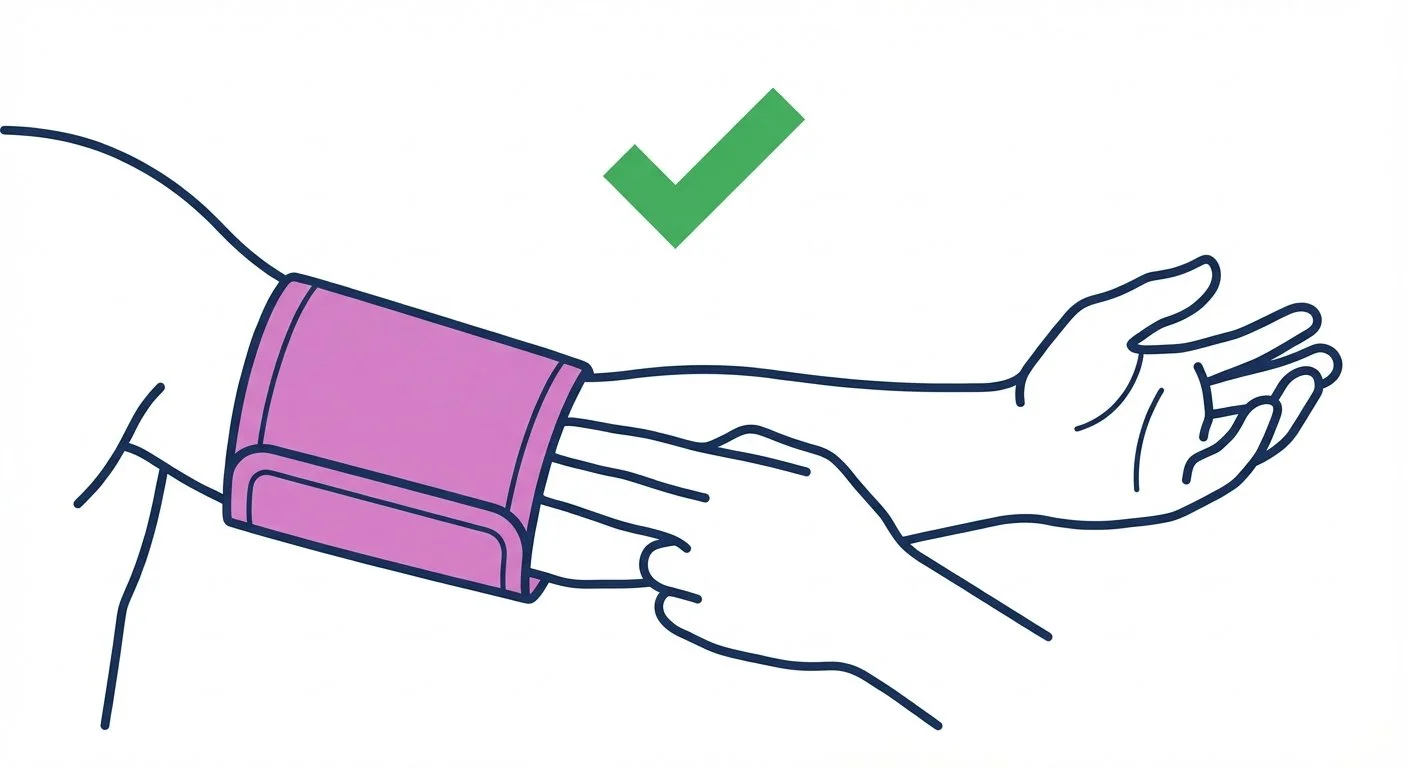
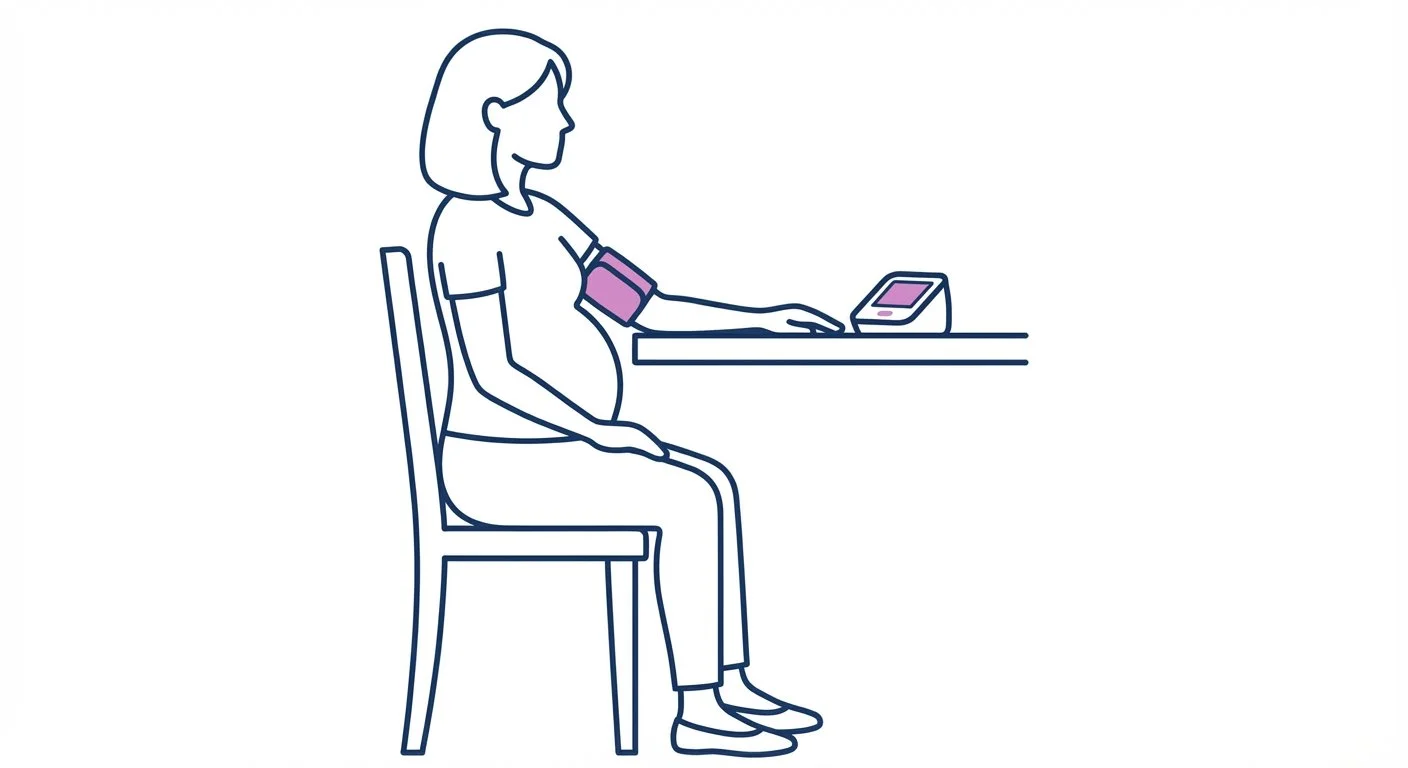
Position the Cuff
Place the cuff on bare skin — not over clothing
Bottom edge about 1 inch above your elbow crease
Tubing runs down the inside of your arm
Check the fit before you start:
Two fingers fit comfortably under the cuff = good fit
Room for 3–4 fingers = too loose, tighten it
Barely fits 1 finger = too tight, loosen it
If adjusting doesn't help, you may need a different cuff size. Ask your provider or pharmacist.
Take Your Reading
Stay still and quiet — no talking, no scrolling, no distractions
Take 2–3 readings, at least 1 minute apart
Breathe slowly and naturally between readings
Record every reading with the date, time, and which arm you used
Aim for the same time each day. Morning readings — before eating or taking medication — tend to be the most consistent. But any consistent time is better than a random one.
If your first reading is above 140/90: Don't panic. Rest for a few minutes, then take another reading. One elevated number is information, not an emergency. It means you need more data — and that's exactly what you're gathering.
After Your Reading
Your care team may set personalized targets for you. The thresholds below are general guidelines used by most providers during pregnancy. Always follow the specific numbers your provider has set for you.
Below your target → Continue monitoring on your normal schedule. You're building a picture your care team can use.
Near or above 140/90→ Stay calm. Rest for a few minutes and remeasure. If still elevated, contact your care team or let them know at your next visit. A note about home readings: because home monitors measure in a calmer environment, some providers consider a home reading of 135/85 equivalent to 140/90 in the office. Ask your provider what numbers they want to hear about.
Above 160/110 → Take at least 3 readings to confirm, resting between each. If consistent, contact your care team right away. Do not wait for your next appointment
Warning Signs — At Any Reading
Contact your provider immediately if you experience any of the following symptoms, even if your numbers are at or below your target:
Severe headache that won't go away
Vision changes — blurry vision, seeing spots, or flashing lights
Upper abdominal pain, especially on the right side under your ribs
Sudden swelling in your face or hands
Shortness of breath
Seizure or loss of consciousness
These symptoms matter even if your blood pressure looks normal. Some pregnancy complications — like preeclampsia and HELLP syndrome — can progress quickly. Reporting these symptoms early gives your care team the best chance to protect you and your baby.
If you can't reach your provider and symptoms are severe, go to the emergency room. You are not overreacting. You are doing exactly what you should.
After Delivery: Keep Monitoring
Most guides stop here. But blood pressure complications don't always end when pregnancy does.
Blood pressure often rises again 3–6 days after delivery — even if your numbers were fine during pregnancy.
New-onset preeclampsia can develop up to 6 weeks postpartum. This catches many women off guard because they assume the risk is over.
40% of hypertension-related maternal complications happen postpartum.
What to do:
Continue monitoring at home for at least 6 weeks after delivery, or as long as your provider recommends
Watch for the same warning signs listed above — they apply postpartum too
Attend your postpartum follow-up appointments, even if you feel fine
If you develop new symptoms (headache, vision changes, swelling) in the weeks after delivery, contact your care team right away
Your body is still recovering. Monitoring after delivery is just as important as monitoring during pregnancy.
Tips for Consistent Readings
Same arm, same time, every day. Routine builds reliable data. Pick a time you can stick to.
Record every reading — even the good ones. Your care team needs the full picture, not just the highs. Trends matter more than any single number.
One high reading is not a diagnosis. Patterns over days and weeks are what your provider is looking for. That's why consistent tracking matters.
Don't compare your numbers to someone else's. Pregnancy-specific targets vary by person, trimester, and medical history. Your provider sets yours for a reason.
If you're unsure about a reading, call. You are never bothering your care team by asking. That's what they're there for.
Bring your log to every appointment.** Whether it's a notebook, an app, or a printout, organized readings help your provider make better decisions for you.
You're Doing This Right
Taking your blood pressure at home is one of the most important things you can do for yourself and your baby — during pregnancy and after. It doesn't need to be perfect. It needs to be consistent.
Trust your readings when you follow these steps. Trust your care team to help you understand what they mean. And trust yourself — you're paying attention, and that matters.
Want to track your readings with pregnancy-specific guidance? Join the Connura Waitlist
Want the full guide with detailed explanations? Read: How to Take Your Blood Pressure at Home
For educational purposes only. This information is not medical advice, diagnosis, or treatment. It does not replace your provider's guidance. Always follow your care team's specific instructions for your pregnancy.
